Implementing DevOps in Healthcare: How to do it, Benefits and Challenges
Last Updated on March 31, 2026
Blog Summary
This blog post explores the implementation of DevOps in healthcare, detailing how to get started and highlighting key benefits. It also covers real-world use cases, addresses common challenges, and shares industry-specific best practices tailored to modern healthcare systems.
Table of Contents
The healthcare industry is undergoing a major digital shift, yet many hospitals still operate on legacy infrastructure that hinders innovation, delays updates, and increases security vulnerabilities. To meet rising patient expectations and regulatory demands, organizations are adopting agile methodologies and CI/CD pipelines enabled by DevOps.
A Redgate report reveals that 73% of healthcare organizations have already embraced DevOps to speed up software delivery and improve operational efficiency. This growing adoption reflects a broader industry shift, as the global healthcare cloud computing market is projected to grow from $53.8 billion in 2024 to $120.6 billion by 2029, driven by cloud adoption. (source)
As this adoption grows, so does the responsibility to ensure these systems are secure, compliant, and resilient. Healthcare providers are under increasing pressure to uphold HIPAA compliance and safeguard sensitive patient data amidst escalating cyber threats.
DevOps addresses these needs by embedding security early in the development cycle, streamlining workflows, and fostering collaboration between IT, clinical, and compliance teams.
This guide offers a practical roadmap for healthcare leaders, especially CTOs, looking to leverage DevOps to modernize their systems, enhance compliance, and deliver better patient outcomes through faster, safer, and more scalable digital operations.
Nearly 47% of companies use DevOps to accelerate software delivery. This approach plays a bigger role in healthcare, improving systems, boosting efficiency, and enhancing patient outcomes. Here are the key benefits fueling its adoption in the industry.

DevOps enables faster deployment of healthcare applications and portals. It allows providers to offer real-time access to medical records, appointment bookings, and virtual consultations. Patient interaction naturally increases as updates roll out faster and services stay available.
Adopting DevOps in healthcare automates how data is stored, accessed, and shared. Using Infrastructure as Code (IaC) and automation tools ensures that patient data moves securely across systems, reducing human error and improving the accuracy of regulatory reporting.
DevOps uses CI/CD pipelines to automate building, testing, and deploying code. It shortens development cycles, ensures fewer bugs reach production, and allows continuous delivery of secure and tested updates.
DevSecOps integrates security into every stage of development. By automating security checks and enforcing HIPAA-compliant practices like access logging and encryption, healthcare systems stay protected and audit-ready.
DevOps improves collaboration across development, operations, QA, and security teams. In healthcare, this helps IT and clinical tech teams work together more effectively, leading to faster issue resolution and better alignment with business goals.
By automating infrastructure and deployments, adopting DevOps in healthcare reduces manual work and lowers operational costs. Healthcare organizations can reinvest these savings into patient care, medical innovation, or staff development.
Continuous testing and monitoring in DevOps improve software quality. This results in more stable healthcare applications, fewer outages, and reduced medical errors due to software glitches.
Healthcare organizations using DevOps practices can leverage autoscaling and cloud-native tools to stay responsive during high-traffic situations. Implementing DevOps in healthcare ensures systems can scale smoothly without downtime, even during pandemics or seasonal surges.
DevOps practices support gradual and monitored system migrations. Legacy healthcare systems can move to cloud or modern infrastructure in phases, minimizing risk and ensuring zero downtime during transitions.
At its core, DevOps for healthcare enables better software delivery, faster EHR systems, more stable patient apps, and smarter diagnostics tools. These improvements lead to smoother clinical workflows, shorter wait times, and better overall patient outcomes.
Explore our Healthcare IT Services designed to help providers automate workflows, improve data security, and scale infrastructure without compromising patient care.
Below are real-world examples of how using DevOps in healthcare is improving speed, enhancing security, and streamlining service delivery across the industry.
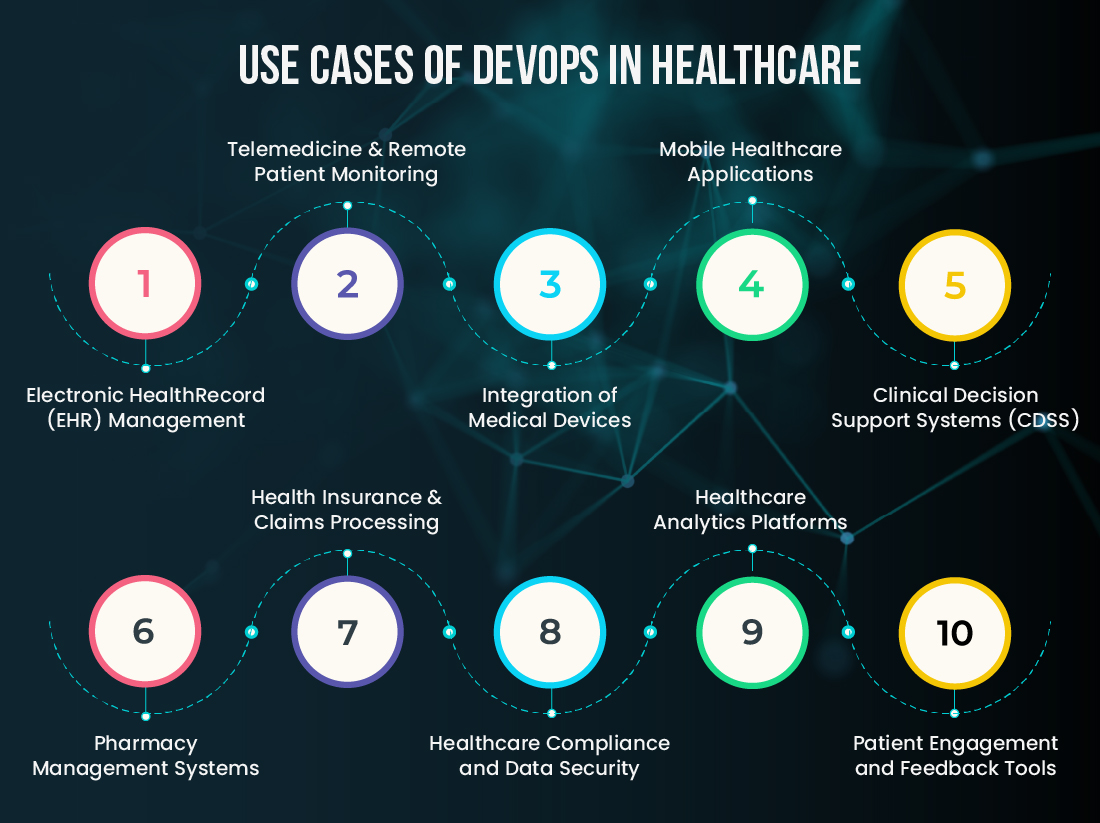
Managing EHR systems is critical but challenging due to constant regulatory updates and usability demands. DevOps helps automate testing and deployment of updates, ensuring EHR systems remain secure, compliant, and accessible at all times, with minimal disruption to clinical workflows.
Telehealth platforms require ongoing improvements to meet the growing demand for virtual care. DevOps supports continuous delivery, allowing quick rollout of new features, video consultation enhancements, and secure data exchange, ensuring a smooth experience for both patients and healthcare providers.
Hospitals use a wide range of connected devices for monitoring and diagnostics. DevOps helps automate the deployment and validation of firmware and software updates for these devices, ensuring they integrate smoothly with existing hospital systems and meet DevOps compliance standards.
Apps for scheduling, reminders, and health tracking must stay up to date and secure. DevOps enables fast release cycles, frequent bug fixes, and real-time updates, improving mobile app performance and patient engagement without compromising data privacy.
CDSS tools offer doctors evidence-based recommendations during patient care. DevOps supports regular improvements to these systems by automating updates to logic, algorithms, and user interfaces, ensuring that clinicians always have timely, accurate decision support.
Managing prescriptions, stock, and regulations requires accurate and stable systems. DevOps helps automate system updates and new feature rollouts, ensuring pharmacies stay compliant, reduce medication errors, and improve inventory efficiency.
Insurance platforms must process claims quickly and accurately. DevOps improves this by streamlining software delivery, reducing processing errors, enabling faster deployment of policy changes or rule updates, and enhancing service reliability and customer satisfaction.
Patient data security is a top priority. DevOps embeds security practices into the development pipeline, running automated scans, monitoring vulnerabilities, and enforcing compliance checks, so that every system change meets healthcare regulations like HIPAA or GDPR.
Analytics systems process large amounts of data to support clinical decisions and resource planning. DevOps ensures these platforms are always up to date, enabling faster delivery of dashboards, smarter algorithms, and scalable infrastructure to support growing data needs.
Platforms that gather patient feedback or send health updates benefit from continuous improvement. DevOps enables healthcare providers to quickly introduce new features, personalize communication, and improve responsiveness, making patient interactions more meaningful and effective.
Getting started with DevOps in healthcare means building fast and secure workflows that deliver updates without risking patient safety or data privacy. It requires careful planning, team collaboration, and smart automation across the DevOps lifecycle. The steps below outline how to begin this process effectively.

Start by creating a DevOps plan that fits your healthcare environment. Go beyond general goals like faster delivery and focus on outcomes like reducing downtime during peak hours, maintaining uninterrupted access to EMRs, and smoothly meeting audit and compliance needs.
Involve doctors, IT staff, and compliance teams early on to ensure that priorities align with healthcare standards like HIPAA and HL7.
A version control system like Git helps teams safely manage code and track every change. In healthcare, it should also track changes to scripts, configuration files, and automation processes.
Connecting each code change to a task or compliance requirement helps teams understand why it was made, meet audit goals, and fix issues faster if problems come up.
Healthcare platforms often rely on multiple interconnected systems, such as billing modules, EHRs, and patient portals. Using containers (like Docker) lets you run each system part separately, making it easier to update features without breaking others.
DevOps orchestration plays a key role in managing these complex environments by coordinating containerized services, infrastructure automation, and deployment workflows. Tools like Terraform help to keep environments consistent, secure, and scalable as patient demands grow.
Continuous Integration (CI) helps developers automatically test and merge code changes into a shared repository. This ensures any problem is found early, before it affects real users.
Implementing DevOps in healthcare requires CI pipelines that check patient data accuracy and perform workflow testing so updates to systems like patient portals or lab results don’t introduce errors.
Automating the build process ensures that every code change is quickly packaged, tested, and consistently ready for deployment. This reduces the chances of human error and speeds up delivery across environments.
In the context of DevOps for healthcare industry, automated builds are especially crucial when updating critical systems like medication tracking or insurance platforms, where accuracy, compliance, and speed are non-negotiable.
Automated testing in DevOps should simulate real clinical workflows, such as scheduling visits, accessing patient records, or submitting claims. They should also include security, compliance, and data handling validations. This ensures that each release is safe, accurate, and meets healthcare standards.
Continuous Deployment (CD) enables faster releases, but updates must be rolled out with strict control in healthcare. Use methods like feature flags or phased rollouts to limit risk. Always have rollback options in case something goes wrong. For example, if an update to a clinical dashboard causes delays, returning to the stable version should be easy.
DevOps monitoring tools help track how apps perform, especially during high-traffic times like early mornings or flu season. Watch key metrics like system response time, login failures, or delays in data updates. Combine technical monitoring with doctors, nurses, and support staff feedback to fix problems quickly and improve the experience for patients and providers.
DevOps challenges such as unstable environments, skill shortages, and tool sprawl are common across industries. However, in healthcare, these challenges are amplified by strict regulatory pressure, data privacy demands, and the critical need for uninterrupted patient care. Have a look at the top DevOps challenges healthcare teams must address:
In healthcare, system downtime can delay treatments, disrupt access to patient records, or interrupt critical services. Even minor outages can impact care and safety. Many DevOps setups lack real-time monitoring or ways to handle failures quickly.
To keep systems stable, teams should add health checks, automatic recovery steps, and safe rollback options to their pipelines. These measures help catch issues early and reduce the risk of service disruptions.
Adopting DevOps into healthcare is not just about using new tools. It also requires a change in mindset, better teamwork, and updated technical skills. Many teams still rely on manual steps or older systems, which makes this shift difficult.
Using a DevOps maturity model can also help healthcare teams assess their current capabilities and set realistic, phased goals. It provides a structured view of where improvements are needed, from cultural alignment to automation readiness, allowing for smoother adoption across departments.
Many healthcare teams focus on basic metrics like uptime or the number of resolved tickets. These numbers may look good, but they don’t show how well the DevOps process works. This can lead to wrong decisions and missed opportunities to improve.
Instead, teams should track DevOps metrics that reflect real progress, such as how often updates are made and how quickly issues are fixed. These insights help improve delivery speed while keeping systems reliable and safe for patient care.
AI is now widely used in healthcare for tasks like patient monitoring, diagnostics, and automating workflows. However, many DevOps pipelines are not designed to support AI models or manage large, sensitive healthcare data. This leads to outdated models, poor results, and risks with data compliance.
To address this, teams should include proper testing, data versioning, and validation steps in their CI/CD pipelines. Connecting AI workflows with DevOps ensures models stay accurate, reliable, and safe to use. It also helps maintain compliance in DevOps for healthcare data protection standards.
Hire DevOps developers who specialize in building secure, scalable pipelines that support AI and data compliance.
The demand for healthcare applications can vary quickly due to emergencies, patient surges, or time-sensitive tasks. Without proper planning, teams may overprovision resources, leading to high cloud costs, or underprovision, which can slow down critical systems.
To avoid this, teams should monitor usage patterns and use autoscaling to adjust resources based on real-time needs, keeping both performance and cost under control.
Patient data is highly sensitive and must be protected at every stage of the DevOps process. However, many teams skip essential steps like securing credentials or scanning code for risks, which can lead to data breaches.
By integrating access controls, automated vulnerability scans, and secret management tools directly into the CI/CD process, teams can reduce the risk of breaches while meeting compliance requirements like HIPAA.
Many healthcare organizations still rely on old systems that are difficult to update or automate. These systems often slow down new releases and require extra effort to maintain; replacing them completely can be costly and risky.
A better approach is to modernize step by step, by slowly moving parts of the system to containers or separating key services, so they can work smoothly with DevOps without causing disruptions.
DevOps in healthcare needs support from more than just IT teams. Doctors, compliance officers, and business leaders also play an important role in how systems are planned and used. If these groups work separately, it can lead to confusion and slow progress.
Building early alignment through joint planning sessions and continuous feedback helps teams stay on track and deliver solutions that serve all stakeholders.
Some healthcare teams jump into DevOps without a clear plan, often due to pressure to modernize quickly. They try too many tools or change everything at once, which leads to confusion and burnout.
For adopting DevOps in healthcare, the best way is to start with small, low-risk projects that allow teams to learn, refine processes, and scale confidently while minimizing operational risks.
To implement DevOps for healthcare successfully, teams must follow key best practices that ensure speed, security, and compliance, without compromising patient care.
Begin by automating critical workflows using DevOps tools, such as test automation or deployment for patient-facing applications. This helps reduce manual errors, speeds up release cycles, and builds confidence in DevOps without disrupting essential services.
IaC ensures that infrastructure across development, testing, and production environments is consistent and repeatable. For healthcare, this means fewer configuration drifts, lower chances of service outages, and better compliance with infrastructure-related policies.
Security in healthcare can’t be an afterthought. Adopt a DevSecOps approach to ensure security checks are integrated at every phase of development, from code scanning to vulnerability assessments, to protect sensitive patient data and meet regulations like HIPAA or GDPR.
Healthcare projects often involve multiple domains: doctors, developers, compliance experts, and support staff. Cross-functional teams promote shared ownership and faster feedback, ensuring that tech solutions align with clinical and operational needs.
Downtime or performance lags can directly affect patient care. Use real-time monitoring tools to track application health, system load, and user experience, so issues can be detected and resolved before they disrupt care delivery.
In healthcare, security cannot be treated as a final step before release. It has to be part of every stage of your development pipeline.
DevSecOps shifts compliance left by integrating security checks, automated testing, and policy enforcement from the start of development. This helps healthcare teams stay audit-ready without adding any complications to their release process.
Healthcare software manages some of the most sensitive data in any industry, including patient records, diagnostics, and billing history. A single breach does not just carry financial consequences. It damages patient trust and brings serious regulatory penalties.
According to IBM’s Cost of a Data Breach Report 2024, healthcare has recorded the highest average breach cost of any industry for 13 consecutive years, reaching $9.77 million per incident.
Here are the five compliance frameworks every healthcare service provider is expected to meet:
1. HIPAA (US): Protects patient health information (PHI) across storage, transmission, and access. Non-compliance penalties range from $100 to $50,000 per violation, based on how the violation occurred and whether it was preventable.
2. GDPR (EU): Applies to any system handling EU patient data. It covers consent management, data residency, and the right of patients to request their data to be deleted. Fines can reach €20 million or 4% of annual global turnover.
3. ISO 27001: A globally recognized security management standard. Healthcare organizations use it to show clients, insurers, and regulators that their data protection practices meet a defined benchmark.
4. FDA 21 CFR Part 11: Governs electronic records and signatures in pharmaceutical and medical device software. It is essential for teams building clinical trial platforms or regulated SaaS products.
5. SOC 2 Type II: A standard requirement for healthcare SaaS vendors. It confirms that data security controls are in place and working continuously, which enterprise buyers check during procurement.
Traditional compliance in healthcare depends on manual audits and end-of-cycle reviews. Security checks create bottlenecks, and teams scramble to fix gaps before certification deadlines. DevSecOps turns compliance into an automated, continuous function inside your CI/CD pipeline rather than a separate process.
Have a look at how it handles each part:
By implementing DevSecOps in Healthcare, teams can ship updates faster and stay audit-ready without compliance becoming a regular problem.
Hire DevSecOps engineers from Bacancy and build a compliant, automated security pipeline that protects patient data at every stage of development.
Implementing DevOps in healthcare is not just a trend. It is a significant shift that is improving how healthcare organizations build, manage, and deliver technology. From reducing downtime during peak hospital hours to enabling safer and faster software updates, DevOps helps teams respond better to patient needs while meeting high standards for compliance and security. Partnering with experienced DevOps consulting company can help tailor this transformation to your organization’s unique needs.
By adopting DevOps, healthcare providers can streamline their development cycles, detect issues early, and deploy changes with reduced risk. It also supports stronger collaboration between IT, compliance, and clinical teams, ensuring that each update improves both care delivery and operational efficiency.
By adopting DevOps for healthcare, providers gain faster app delivery, better system stability, and improved collaboration between IT and clinical teams. This leads to enhanced patient experiences and operational efficiency.
DevOps streamlines software delivery, reduces downtime, and improves system reliability. It enables faster updates to EHRs, telehealth platforms, and other healthcare tools, directly improving patient care and operational efficiency.
Yes, especially with DevSecOps. Security is integrated throughout the development lifecycle with practices like code scanning, access control, and compliance checks, helping protect sensitive patient information and meet HIPAA or GDPR requirements.
Yes. DevOps pipelines can integrate AI workflows by adding steps like model testing, data validation, and version control. This ensures AI tools in diagnostics or monitoring stay accurate and compliant.
DevOps supports healthcare compliance by making every release traceable and audit-ready. CI/CD pipelines log what changed, when, and by whom. Automated testing catches issues before they reach production, and compliance updates ship on schedule instead of waiting on manual reviews.
DevOps focuses on streamlining development and operations through automation and collaboration. DevSecOps takes it a step further by embedding security and compliance checks at every stage of the pipeline, making it especially well-suited to the high-stakes regulatory environment of healthcare.
Your Success Is Guaranteed !
We accelerate the release of digital product and guaranteed their success
We Use Slack, Jira & GitHub for Accurate Deployment and Effective Communication.