Quick Summary:
This blog covers 11 practical tips to ensure data privacy in healthcare while embracing artificial intelligence. Learn how to manage hidden risks, control costs, and maintain compliance as AI becomes a core part of your healthcare systems.
Table of Contents
Introduction
Over 190 Million Health Records were exposed in a single breach: Is your system really safe?
AI is making healthcare smarter, faster, and more connected. However, as advanced technology quietly becomes part of diagnoses, records, and patient care, it also brings serious risks.
All it takes is one unapproved AI tool and an old test database to expose patient data.
This blog shares 11 practical ways to strengthen data privacy in healthcare, manage risks like shadow AI and shadow data, and prepare your healthcare systems to stay secure while moving forward with AI.
If you work in healthcare tech or handle patient records, this guide on data privacy in healthcare in the era of artificial intelligence offers clear insights and practical steps to help you stay compliant, secure, and in control.
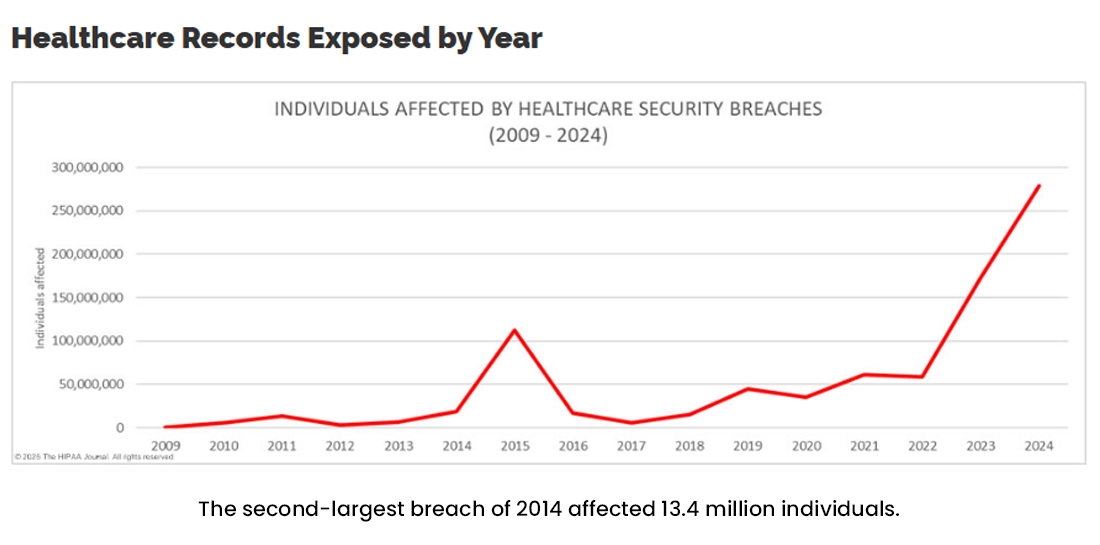
Source: Hipaa Journal
Why Data Privacy in Healthcare Needs a Rethink in the Age of AI?
Data privacy and security in healthcare have become a serious concern in the era of Artificial Intelligence. The integration of AI into EHRs, patient monitoring, diagnostics, and even billing has provided incredible innovation, but it has also opened up new and complex security risks.
According to the report, with a population of 341 million people, the breach affected 1 in 2 Americans. That’s an enormous number of people exposed, with sensitive medical details potentially falling into the wrong hands. And the risks are only accelerating.
A recent study by the IBM Institute for Business Value revealed that only 24% of current-gen AI projects include built-in security, even though 82% of executives believe that secure and trustworthy AI is essential to business success.
Shockingly, the same study shows that 70% of people prioritize innovation over data protection, which indicates short-term gains often come at the cost of long-term risk and a trade-off that can cost millions.
Further, nearly 40% of breaches involve data stored across multiple environments, especially in hybrid cloud infrastructures. Breached data stored in public clouds now carries the highest average cost at $5.17 million per incident.
Let’s take a reality check- straight from the frontlines of global healthcare.
This isn’t just a one-country problem; the concern about healthcare data privacy is worldwide.
- 40% of doctors in the USA are uneasy about how AI is being used to manage patient data.
- In the UK, 84% of healthcare professionals say they’ve experienced at least one data breach since 2023.
- A survey in Asia found that 33% of medical professionals are concerned about patient privacy when adopting AI in their practice.
- A global study of 1,450 healthcare IT professionals across the U.S., Canada, Europe, and Asia found growing tension between AI adoption and the lack of strong security policies.
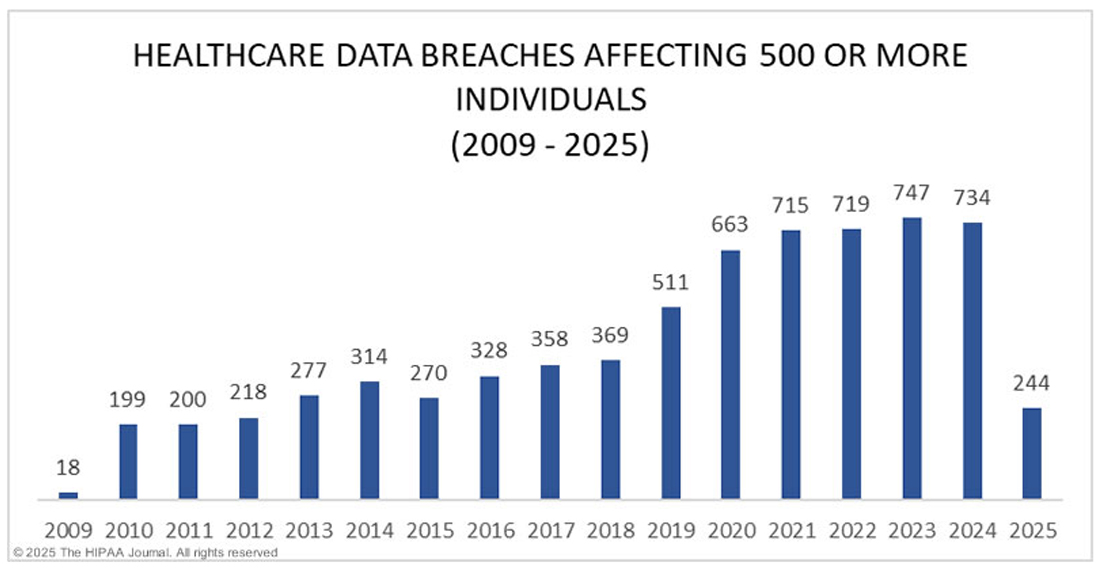
Source: Hipaa Journal
The risks and concerns are real; however, they’re not unbeatable. Let’s walk through 11 proven strategies to protect your sensitive patient data without slowing down innovation.
11 Tips to Ensure Healthcare Data Privacy with AI
From 2018 to 2024, the Health and Human Services (HHS) reported a 264% increase in large ransomware breaches, and 7 health systems had been fined up to $950,000 for failing to protect patients’ protected health information from ransomware attacks.
Now, with Artificial Intelligence (AI) joining the mix, things have become even riskier. AI is amazing for making things fast and efficient with its smart automation. However, if privacy and security aren’t built in right from the start, AI can actually make these vulnerabilities much bigger.
As recent reports and Reddit discussions clearly show, healthcare data privacy breaches are a serious problem. But don’t worry; you can still protect your data.

Here are 11 tried-and-tested tips that will help you create a secure, trustworthy, and compliant healthcare solution.
1. Implement Strong Data Governance Policies
2. Adopt Encryption and Anonymization Techniques
3. Ensure Compliance with HIPAA, GDPR, and Local Regulations
4. Build AI Models Using Privacy by Design
5. Limit Data Collection to What Is Necessary
6. Use Secure Cloud Storage and Infrastructure
7. Monitor and Log Data Access
8. Conduct Regular Risk Assessments
9. Educate Staff and Stakeholders
10. Appoint a Chief Privacy or Security Officer
11. Plan for Data Breaches with a Response Strategy
1. Implement Strong Data Governance Policies
Data governance means you have clear rules on who owns it, has access to it, and manages it. In the healthcare industry, every privacy safeguard begins with governance. Also, by implementing data governance, you can define your data ownership, data lifecycle management, and auditability.
What You Can Do:
- Appoint data stewards to oversee sensitive data types like Protected Health Information (PHI) and electronic Protected Health Information (ePHI).
- Build automated audit trails that log who accessed what, when, and why.
- Include governance checkpoints in every product update or data flow change.
- Align your governance model with NIST’s (National Institute of Standards and Technology) data classification standards.
2. Adopt Encryption and Anonymization Techniques
You might have heard about end-to-end encryption on your mobile devices; similarly, in healthcare, encryption is crucial to protect data at rest and in transit. With anonymization or tokenization, you can ensure the data is accessible and cannot be easily traced by an unauthorized person.
It also decreases exposure during analytics, training, or research, supporting strong data privacy and security in healthcare.
What You Can Do:
- Implement AES-256 for database encryption and TLS 1.3 for data in transit.
- Apply tokenization for identifiers like medical record numbers, date of birth, and insurance numbers.
- Adapt pseudonymization for AI/ML datasets to balance utility and privacy.
- Encrypt backup files, not just live systems. Breaches often happen via backups.
3. Ensure Compliance with HIPAA, GDPR, and Local Regulations
A common assumption every healthcare provider has is that HIPAA compliance is insufficient. You must also consider GDPR, DPDPA (India), and emerging AI health laws. Most importantly, you are subject to local privacy regulations, but each has strict patient consent and breach reporting requirements.
You can also get in touch with a HIPAA compliance services provider who can provide you with the proper regulation checklist and expertise on the regulations.
What You Can Do:
- Build a compliance matrix that tracks applicable laws by region and data type.
- Automate data subject rights (DSR) workflows like access, deletion, and portability.
- Utilize privacy management platforms to manage consent and opt-outs at scale.
- Localize storage for jurisdictions with data residency laws (e.g., India DPDPA).
4. Limit Data Collection to What Is Necessary
Every extra piece of data you collect increases your liability without improving outcomes. Healthcare data is quite sensitive, and collecting it beyond the required level inflates your exposure and violates standards like HIPAA’s Minimum Necessary Rule. It also violates key compliance standards.
What You Can Do:
- Review all required forms, APIs, and device inputs.
- Avoid storing full Social Security Numbers (SSN), birth dates, or addresses unless it’s critical.
- Segment optional data fields from mandatory ones in your EHR or app forms.
- Build privacy by design right into your intake and onboarding flows.
5. Use Secure Cloud Storage and Infrastructure
A generic cloud hosting might offer basic security, but it does fall short of the stringent requirements set by HIPAA, HITRUST, GDPR, and local data protection laws like India’s DPDPA. Healthcare data demands specialized encryption, logging, and access control. Any gap in compliance can expose your organization to fines and loss of patient trust.
What You Can Do:
- Choose providers that offer BAA (Business Associate Agreements) and HITRUST certifications.
- Use pre-configured HIPAA-compliant environments like AWS HealthLake or Azure for Healthcare.
- Adopt encryption, secure identity management, and audit logging by default.
- Limit PHI storage to regions with strong health data laws if operating globally.
6. Build AI Models Using Privacy by Design
AI adds immense value to diagnostics, personalization, and automation, but if it learns from raw patient data, it becomes a privacy risk. Whether you are developing predictive tools, patient engagement platforms, or diagnostic support systems, any data flowing through these models needs to be secured.
In the healthcare industry, where data includes electronic health records (EHRs), clinical notes, imaging files, lab results, and even genomic information, one small exposure can lead to major violations of trust and law. A reputable EHR development company will embed privacy-by-design principles from the outset.
What You Can Do:
- Implement federated learning to train models without centralizing PHI.
- Use privacy-preserving machine learning (PPML) like differential privacy.
- Maintain data provenance logs to track data flow from source to model output.
- Run regular AI audits to assess for model leakage and bias.
7. Implement Monitor and Log Data Access
In healthcare, delayed breach detection can cost more than you think. It is often the only thing that distinguishes between a contained incident and a massive breach. A real-time monitoring helps you detect suspicious behavior before the case escalates.
For instance, if someone accesses protected health information at an unusual time, from an unknown device, or repeatedly, you should know instantly.
What You Can Do:
- Set up SIEM (Security Information and Event Management) tools to log every action.
- Automate alerts for suspicious data access, bulk downloads, or failed logins.
- Utilize behavioral analytics to detect unusual usage patterns in real time.
- Retain logs long enough to support compliance investigations and audits.
8. Conduct Regular Risk Assessments
Every time you introduce a new integration, be it a third-party chatbot, a wearable device, or a telemedicine module, you change how patient data flows, which opens up new risks. Privacy Impact Assessments (PIAs) help you assess, document, and mitigate these risks before it’s too late.
What You Can Do:
- Perform PIAs for every new feature that touches patient data.
- Assess risk for all third-party tools, including CRMs and AI APIs.
- Make PIAs a mandatory step in your SDLC (Software Development Lifecycle).
- Document outcomes and mitigation strategies in case of an audit.
9. Educate Staff and Stakeholders in Privacy and Security Awareness
Even the best infrastructure can be damaged by silly human error. Several healthcare breaches were initiated by innocent mistakes, like a staff member accidentally clicking a phishing link, sending PHI over email, or using weak passwords. Hence, a technology breach can cause massive errors if your people aren’t trained.
What You Can Do:
- Run quarterly privacy and phishing awareness training.
- Simulate real attacks and test employee readiness.
- Educate developers on secure coding and data minimization.
- Make privacy part of your culture, not just compliance.
10. Appoint a Chief Privacy or Security Officer
A single point of accountability is crucial. This role ensures data privacy isn’t just a legal boilerplate but part of daily operations. A dedicated officer brings focus, accountability, and strategy to your data protection efforts. It will also efficiently maintain data privacy and security in healthcare.
What You Can Do:
- Appoint a senior-level privacy or security officer, even for some time.
- Have them lead audits, privacy design reviews, and vendor evaluations.
- Ensure they report directly to leadership, not just the engineering chain.
- Encourage cross-functional alignment across product, legal, and compliance.
11. Plan for Data Breaches with a Response Strategy
A data privacy breach is no longer a question of if; it’s a question of when. Being unprepared only makes it worse and creates chaos that will be hard to handle at some point. You need a documented plan with timelines, roles, and action items.
What You Can Do:
- Create a detailed incident response plan (IRP); don’t wait for it until after a breach.
- Define roles like who contacts regulators, patients, legal, and internal teams.
- Practice with mock breach simulations at least twice a year.
- Keep your plan updated as systems, teams, or regulations evolve.
Ready to Develop Regulation-Ready Healthcare Systems?
Hire EHR developers and build intelligent healthcare systems that are designed to be secure, compliant, and privacy-first!
Know About Shadow AI and Shadow Data - The Hidden Risk in Data Privacy

Every healthcare organization has strong encryption, clear compliance checklists, and even a breach plan in place. Still, if you are not aware of Shadow AI and Shadow Data, your system may already be vulnerable from the inside.
Shadow AI refers to artificial intelligence tools or models deployed without official oversight from your IT, data privacy, or compliance teams. They might be experimental features, quick integrations by individual teams, or third-party AI APIs running on patient data without formal security checks.
Whereas Shadow Data includes duplicate, residual, or forgotten data stored in caches, logs, testing environments, or obsolete backups. It often lives outside your regular governance or monitoring systems, which makes it a prime target for attackers.
In fact, 1 in 3 data breaches now involve shadow data, which highlights how the uncontrolled sprawl of information is becoming one of healthcare’s biggest blind spots.
Where Problems Hide:
➜ AI tools used without oversight might leak or memorize sensitive patient information. That’s a direct privacy violation.
➜ Old test data, forgotten backups, and temporary files can persist longer than they should, unencrypted and untracked.
➜ The most costly breaches in data privacy and security in healthcare often come from places your security team didn’t even know existed.
Practical Ways to Fix the Risk:
Run deep data audits regularly; don’t just check what’s obvious, but scan what’s forgotten.
Set rules around AI usage, such as what tools are allowed, who approves them, and how they handle data.
Create AI sandboxes that are safe for testing yet cut off from real patient information.
You can utilize tools that flag unauthorized AI apps being used inside your organization.
Don’t let data live forever in your system; eliminate what’s outdated, useless, or redundant on a set schedule.
Understand Data Privacy Laws: A Global Overview
Data privacy laws are legal/regulatory frameworks designed to protect individual, personal, and sensitive information from misuse, unauthorized access, and exploitation. These laws set clear rules on how organizations collect, store, process, and share data.
As digital platforms and AI systems grow more data-intensive, data privacy and security in healthcare regulations ensure the ethical handling of data, safeguard user rights, and promote transparency and accountability in data-driven ecosystems.
Key Global Data Privacy Laws and Regulations You Must Know:
1. General Data Protection Regulation (GDPR) – European Union
Enforced in 2018, GDPR is one of the strictest data protection laws globally. It gives EU citizens control over their personal data and requires organizations to follow transparent data processing practices. If it is violated, then heavy fines can be up to €20 million or 4% of global turnover.
Important guidelines include:
- Data subject rights, access, correction, and deletion
- Consent-based data collection
- Data breach notification within 72 hours
Applies to- All 27 EU member states + European Economic Area (EEA) countries, like Norway, Iceland, Liechtenstein
2. Health Insurance Portability and Accountability Act (HIPAA) – United States
HIPAA governs the privacy and security of PHI in the healthcare sector. It establishes national standards to secure electronic health data and ensure patient confidentiality across digital systems. It can be done through administrative, physical, and technical protection requirements.
Important guidelines include:
- The Privacy Rule regulates the disclosure of PHI.
- Security Rule enforcing safeguards for electronic PHI.
- Mandatory breach notifications to affected individuals and regulators.
Applies to- Healthcare providers, health plans, healthcare clearinghouses, and business associates handling Protected Health Information in the U.S.
3. California Consumer Privacy Act (CCPA) – United States
CCPA grants California residents greater control over their personal data. It is applicable to businesses that handle large volumes of consumer data or meet certain revenue thresholds.
Important guidelines include:
- Right to know, delete, and correct personal data.
- Right to opt out of data selling and sharing.
- Clear privacy notices and consent mechanisms.
Applies to- For-profit businesses that collect personal data of California residents and meet one or more of the following:
➜ Annual gross revenue over $25 million
➜ Buys, receives, or sells data of 100,000+ consumers
➜ Derives 50% or more of revenue from selling personal data
4. Personal Data Protection Bill (PDP) – India
This law is quite famous as the Digital Personal Data Protection Act (DPDP) 2023. India’s law seeks to protect digital personal data and applies to entities processing data within and outside India if it involves Indian citizens.
Important guidelines include:
- Data fiduciaries must process data fairly and lawfully.
- Consent is central to lawful processing.
- Emphasis on accountability and grievance redressal mechanisms.
Applies to- Any organization processing the personal data of individuals in India, whether operating within India or abroad.
5. Privacy Act – Australia
This Act regulates how Australian government agencies and businesses handle personal data. It outlines responsibilities for collecting, storing, and disclosing personal information while ensuring individuals can access and correct their data.
Important guidelines include:
- Open and transparent data management practices.
- Individual rights to access and correct personal data.
- Secure handling and breach notification obligations.
Applies to- Australian Government agencies, private sector organizations with annual turnover, and any business trading in personal information.
Other Notable Global Data Privacy and Security in Healthcare Laws You Should Know
| Law/Regulation | Country/Region | Highlights | Applies to |
|---|
| PIPEDA (Personal Information Protection and Electronic Documents Act)
| Canada | Governs how private-sector organizations collect, use, and disclose personal data in commercial activities
| Private-sector organizations
|
| LGPD (Lei Geral de Proteção de Dados)
| Brazil | Brazil’s equivalent to GDPR requires consent, breach notification, and DPOs | Any organization handling the personal data of Brazilians |
| PDPA (Personal Data Protection Act) | Singapore, Thailand, Malaysia | Leading privacy laws in Southeast Asia focus on consent, access, and usage limits | Businesses, public agencies, and data intermediaries |
| New Zealand Privacy Act 2020 | New Zealand | Introduces mandatory breach notifications and tighter cross-border data handling rules | Government and private-sector entities |
| PIPL (Personal Information Protection Law) | China | One of the most stringent laws, GDPR-like, but includes strict data localization and government oversight | All companies processing Chinese citizens’ data |
| POPIA (Protection of Personal Information Act) | South Africa | Ensures data is processed lawfully and minimally while granting individuals access, correction, or deletion rights | Public and private bodies handling personal information |
How Does Bacancy Help You Maintain Data Privacy in Healthcare in the Era of Artificial Intelligence?
Balancing innovation with data privacy isn’t easy, especially in healthcare, where every decision impacts real lives. As AI becomes part of everyday care, the systems behind it need to be smarter and safer than ever.
At Bacancy, we understand the stakes. As an experienced healthcare web development company, our team enables you to embed privacy into every layer of your digital solution, whether it’s AI-driven diagnostics, EHR systems, or patient portals.
Our development process includes continuous security audits, threat modeling, and integrating AI ethics guidelines to protect patient data from model vulnerabilities and biases.
We have helped healthcare startups, hospitals, and enterprise healthtech providers build HIPAA-compliant platforms that scale effectively. Our healthcare team worked with forward-thinking healthcare professionals to develop AI-powered web platforms that are compliant, secure, and scalable.
Frequently Asked Questions (FAQs)
Data privacy in healthcare means fully protecting sensitive patient data. It ensures proper use under legal boundaries and blocks any unauthorized access or exposure. Laws like HIPAA in the U.S. and similar global regulations set the rules.
Protecting patient data builds trust, prevents identity theft, and ensures compliance with regulations like HIPAA and GDPR. Inaccurate or leaked information can harm patients, damage reputations, and lead to heavy financial penalties.
Key risks include cyberattacks, insider threats, misconfigured cloud storage, outdated legacy systems, and unmonitored AI tools. Shadow data and unauthorized access points often go unnoticed and make your healthcare systems a prime target.
The main types of healthcare data privacy include:
Physical privacy protects patients in physical settings, like private rooms and secure record storage.
Informational privacy ensures medical data is accessed and shared securely.
Decisional privacy is about respecting patients’ rights to choose their data use and care.
Sensitive healthcare data, such as medical history, diagnoses, and treatment records, helps ensure accurate care. It builds patient trust and supports legal compliance. Any misuse may cause identity theft, errors, or legal trouble.







